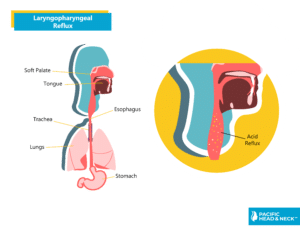
Laryngopharyngeal Reflux is a condition where acid from the stomach affects the throat. Acid travels up from the esophagus (swallowing tube) and gets to the throat.
Diagnosis
Laryngopharyngeal reflux (LPR) is diagnosed by a thorough history of the patient’s symptoms and general health, as well as examination of the throat and voice box using a fiberoptic scope (a very small, lighted flexible tube that is passed through the nose to view the throat and voice box). Traditionally, the diagnosis was also based on the patient’s response to a trial of treatment with acid-suppression medications and reflux precautions through diet and lifestyle changes. However, we now understand that some patients require high-dose therapy (often two to four times the dose routinely recommended for gastro-esophageal reflux disease) for prolonged periods of time. Surgery to control reflux may be recommended in some patients who don’t respond to medications.
Pacific Head & Neck is one of the few centers in the country to offer a highly sensitive, outpatient diagnostic test (Restech Dx-pH Measurement system) to quantitatively measure the degree of reflux into the throat. This is a simple, comfortable test performed with a small probe containing a senor at the tip. It is passed through the nose until the tip is at the back of the throat (high enough that patients cannot feel it when speaking or swallowing). The probe wirelessly records the acid exposure (every 30 seconds) over a 24-hour period. Patients can eat normal meals, go to work and even exercise during the testing period. With the patient’s input, the Dx-System tracks meals, symptoms and supine periods. This helps correlate symptoms and reflux patterns. This is a valuable tool in the comprehensive assessment of patients with laryngopharyngeal reflux.
Diagnosis may also be:
- Acid Reflux:
- Gastroesophageal reflux disease (GERD) and laryngopharyngeal reflux (LPR), commonly known as acid reflux, are acute or chronic conditions associated with frequent heartburn, cough, throat clearing, dysphagia or difficulty swallowing, dyspnea or difficulty breathing, choking and/or hoarseness.
- GERD:
- GERD occurs when acidic content from the stomach regurgitates, or refluxes, into the esophagus, larynx or trachea causing inflammation or damage to these structures. The cause of GERD is unknown, but doctors believe it is the result of multiple factors, including abnormal movement in the lower esophageal sphincter and a hiatal hernia. Heartburn, nausea and difficulty swallowing are common symptoms of GERD, while ulcers, asthma and esophageal cancer can also occur in severe cases. Some patients with GERD may also experience LPR.
- LPR:
- During laryngopharyngeal reflux (LPR), the contents of the stomach and upper digestive tract may reflux all the way up the esophagus, beyond the upper esophageal sphincter (a ring of muscle at the top of the esophagus), and into the back of the throat and possibly the back of the nasal airway. 80% of patients presenting with this condition do not report heartburn. Laryngopharyngeal reflux occurs as acid from the stomach rises to the esophagus and enters the back of the throat. Patients suffering from LPR often report a bitter taste in their mouth, hoarseness and the feeling that mucus or phlegm is caught in the back of their throat. A more uncommon symptom is difficulty breathing, which occurs because the acidic, refluxed material comes in contact with the voice box (larynx) and causes the vocal cords to close to prevent aspiration of the material into the windpipe (trachea). LPR may also be a contributing factor in the development of laryngeal cancer. Women, men, infants, and children can all have LPR, which may result from physical causes or lifestyle factors. Physical causes can include a malfunctioning or abnormal lower esophageal sphincter muscle (LES), hiatal hernia, abnormal esophageal contractions, and slow emptying of the stomach. Lifestyle factors include diet (chocolate, citrus, fatty foods, spices), destructive habits (overeating, alcohol and tobacco abuse) and even pregnancy. Young children experience GERD and LPR due to the developmental immaturity of both the upper and lower esophageal sphincters. It should also be noted that some patients are just more susceptible to injury from reflux than others. A given amount of refluxed material in one patient may cause very different symptoms in other patients.LPR can result in significant throat and laryngeal inflammation, and lead to subglottic stenosis (narrowing of the windpipe below the vocal cords) and lesions such as laryngeal ulcers and granulomas. Chronic, untreated reflux into the throat is now considered a small risk factor for laryngeal cancer. Prompt diagnosis and treatment of LPR is hence critical.